Endometriosis Symptoms & Diagnosis: Your Guide to Treatment Options
Endometriosis is a complex and often debilitating condition affecting millions worldwide. It's a journey many embark on, seeking answers, relief, and often, a cure. The core of this journey often begins with a pressing question:
"La Endometriosis Se Cura?" (Can endometriosis be cured?). While the simple answer is no – there is currently no definitive cure for endometriosis – understanding its symptoms, diagnosis, and the diverse range of available treatments is crucial for effectively managing the condition and improving quality of life. This comprehensive guide aims to shed light on this intricate disease, empowering you with knowledge and actionable insights.
Understanding Endometriosis: When Uterine-Like Tissue Grows Astray
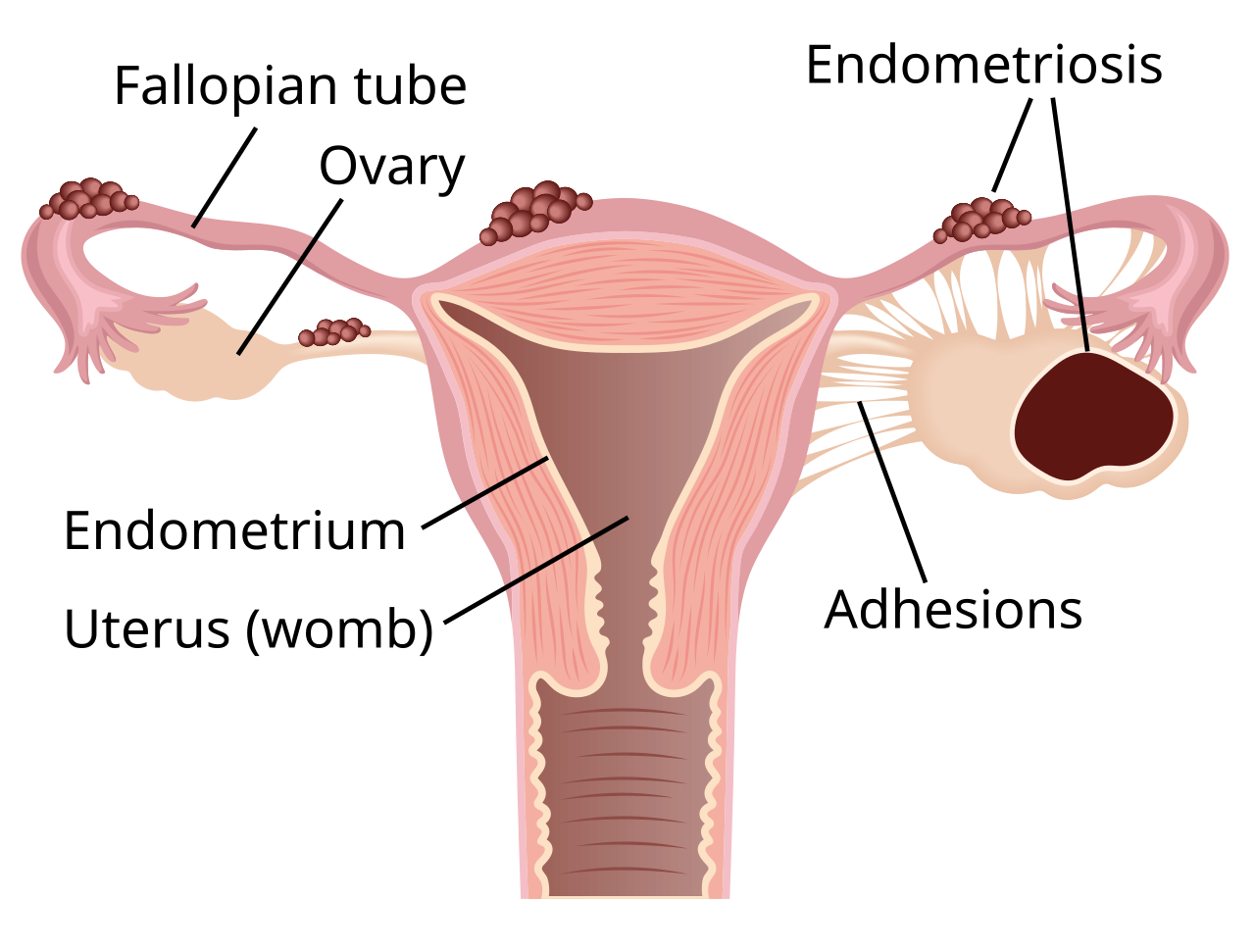
At its heart, endometriosis is a chronic condition where tissue similar to the lining of the uterus – known as the endometrium – grows outside the uterus. These displaced patches of tissue, often referred to as "implants," "nodules," or "lesions," behave much like the uterine lining. They respond to hormonal changes during the menstrual cycle, thickening, breaking down, and bleeding. However, unlike the uterine lining, which exits the body during menstruation, this displaced tissue has no way to escape. This leads to inflammation, pain, scar tissue formation, and adhesions, where organs stick together.
While the exact cause of endometriosis remains unknown, it's believed to be a combination of genetic, immunological, and environmental factors. What we do know is where these rogue tissues most commonly appear:
- On or under the ovaries
- In the fallopian tubes, which carry eggs from the ovaries to the uterus
- Behind the uterus
- On the tissues that hold the uterus in place (e.g., ligaments)
- On the intestines or bladder
In rare instances, these implants can even be found in more distant locations, such as the lungs or other parts of the body, highlighting the widespread potential impact of the disease. This abnormal growth can significantly affect anyone who experiences menstruation, though certain factors can increase or decrease your risk. You might have a higher risk if you have a close relative (mother, sister, daughter) with endometriosis, if your period started before age 11, or if you have short menstrual cycles (less than 27 days) or heavy, prolonged periods lasting more than seven days. Conversely, a history of pregnancy, late onset of periods during adolescence, and breastfeeding are associated with a lower risk.
Recognizing the Signs: Key Symptoms of Endometriosis
The symptoms of endometriosis can vary widely in severity and presentation, making diagnosis challenging. Some individuals experience severe pain, while others may have no symptoms at all. However, two primary symptoms are most commonly associated with the condition:
- Chronic Pelvic Pain: This pain often correlates with the menstrual cycle but can become constant and debilitating. It may manifest as exceptionally painful menstrual cramps that worsen over time, deep pain during or after sexual intercourse (dyspareunia), or pain in the intestines or lower abdomen.
- Infertility: Endometriosis is a significant cause of difficulty conceiving. The inflammation, scar tissue, and adhesions caused by the disease can obstruct fallopian tubes, interfere with ovulation, or affect the quality of eggs or sperm.
Beyond these primary indicators, other symptoms that can signal the presence of endometriosis include:
- Heavy Menstrual Bleeding: Periods with an unusually heavy flow (menorrhagia)
- Irregular Bleeding: Spotting or bleeding between periods
- Gastrointestinal Symptoms: Painful bowel movements, constipation, diarrhea, or bloating, especially during menstruation. These can often be mistaken for irritable bowel syndrome (IBS).
- Urinary Symptoms: Painful urination or frequent urges to urinate, particularly during your period.
- Fatigue: Persistent tiredness or lack of energy, often linked to chronic pain and inflammation.
It's important to remember that these symptoms can also be indicative of other conditions. Therefore, seeking professional medical advice is paramount for an accurate diagnosis. Keeping a detailed symptom journal, noting when pain occurs, its severity, and any accompanying symptoms, can be incredibly helpful for your doctor.
The Path to Diagnosis: Uncovering the Invisible Disease
Diagnosing endometriosis can be a prolonged and frustrating process, often taking years due to the varied symptoms and the "invisible" nature of the implants. If you suspect you have endometriosis, your healthcare professional will typically begin by discussing your symptoms and medical history in detail. This will likely be followed by a pelvic exam, where your doctor may feel for cysts or nodules related to the condition.
Imaging tests, such as ultrasound or MRI, are often part of the diagnostic journey. These tests can help identify larger implants, cysts (endometriomas) on the ovaries, or deep infiltrating endometriosis. While valuable for ruling out other conditions and indicating the presence of endometriosis,
Understanding Endometriosis: No Cure, But Effective Treatments, these imaging techniques alone cannot definitively diagnose the condition. The gold standard for a conclusive diagnosis remains a surgical procedure.
The most common and definitive surgical method for diagnosing endometriosis is a
laparoscopy. This minimally invasive procedure involves a surgeon making a small incision, typically near your navel. A thin tube equipped with a camera and light, called a laparoscope, is then inserted. This allows the surgeon to visually inspect the pelvic organs for endometriosis implants. During the laparoscopy, the healthcare professional can not only diagnose the condition based on the appearance of these patches of endometrial tissue but can also, in many cases, treat it by removing the visible lesions. This dual approach makes laparoscopy an invaluable tool for both diagnosis and initial treatment.
Navigating Treatment Options: Managing Endometriosis Effectively
While the persistent question of
"La Endometriosis Se Cura?" unfortunately still yields a negative answer in terms of complete eradication, modern medicine offers a robust arsenal of treatments designed to manage symptoms, slow disease progression, and improve quality of life. Treatment plans are highly individualized, tailored to the severity of symptoms, the extent of the disease, and whether the individual is trying to conceive.
1. Pain Management for Mild Symptoms:
For those experiencing mild pain, simple analgesics (pain relievers) can often provide relief. Over-the-counter options like ibuprofen or naproxen can help manage menstrual cramps and general pelvic discomfort. Your doctor may also suggest stronger prescription pain medications if needed.
2. Hormonal Therapies:
Since endometriosis tissue responds to hormonal fluctuations, hormonal treatments are a cornerstone of management, particularly for pain and bleeding. These therapies aim to suppress the growth of endometrial implants by reducing or stopping estrogen production, thereby mimicking menopause or pregnancy.
- Hormonal Contraceptives: If you're not currently trying to get pregnant, hormonal birth control methods such as oral contraceptive pills, hormonal IUDs (intrauterine devices), patches, or vaginal rings can significantly help manage pain and heavy bleeding by regulating or suppressing the menstrual cycle.
- GnRH Agonists and Antagonists: These medications temporarily halt the production of ovarian hormones, inducing a temporary menopause-like state. While highly effective in reducing implant growth and pain, they can cause menopausal side effects (hot flashes, bone density loss) and are typically used for a limited duration. Add-back therapy (small doses of estrogen and progestin) can help mitigate side effects.
- Progestin Therapy: Progestin-only medications (pills, injections, or hormonal IUDs) can help by thinning the endometrial lining and suppressing its growth, thereby reducing pain and bleeding.
If you are actively seeking pregnancy, specific medications and approaches are available that can help manage endometriosis while supporting fertility. Discussing your family planning goals with your doctor is critical in determining the most appropriate hormonal strategy.
3. Surgical Interventions:
When symptoms are severe, or if fertility is a primary concern, surgery may be a viable option. The goal of surgical treatment is to remove or destroy the endometrial implants.
- Excision Surgery (Laparoscopy): As mentioned previously, laparoscopy can also be used for treatment. A skilled surgeon can carefully excise (cut out) or ablate (destroy) the endometrial tissue and adhesions. This can significantly alleviate pain and improve fertility outcomes. However, it's important to note that even after meticulous surgery, endometrial tissue can often regrow over time, necessitating continued medication or further intervention. This highlights why for many, Managing Endometriosis: Solutions for Pain, Fertility & Beyond often requires a multi-pronged approach.
- Hysterectomy: As a last resort, for individuals who have exhausted other treatment options and do not wish to become pregnant in the future, a hysterectomy – the surgical removal of the uterus – may be considered. In some cases, the ovaries are also removed (oophorectomy). While this procedure offers a definitive solution to uterine-based issues and can provide significant relief from endometriosis symptoms, it is a major decision with permanent consequences for fertility.
Deciding on the best treatment path requires a thorough discussion with your healthcare provider, weighing the benefits, risks, and personal goals, especially concerning fertility and long-term symptom management.
Conclusion
Endometriosis is a challenging, chronic condition that demands attention, understanding, and proactive management. While the answer to
"La Endometriosis Se Cura?" remains a disheartening "no," breakthroughs in diagnosis and a wide array of treatment options offer real hope for symptom control and an improved quality of life. If you're experiencing symptoms that suggest endometriosis, advocating for yourself and seeking a comprehensive evaluation from a knowledgeable healthcare professional is the first crucial step. With the right diagnosis and a personalized treatment plan, it is entirely possible to navigate life with endometriosis and find meaningful relief.