Managing Endometriosis: Solutions for Pain, Fertility & Beyond
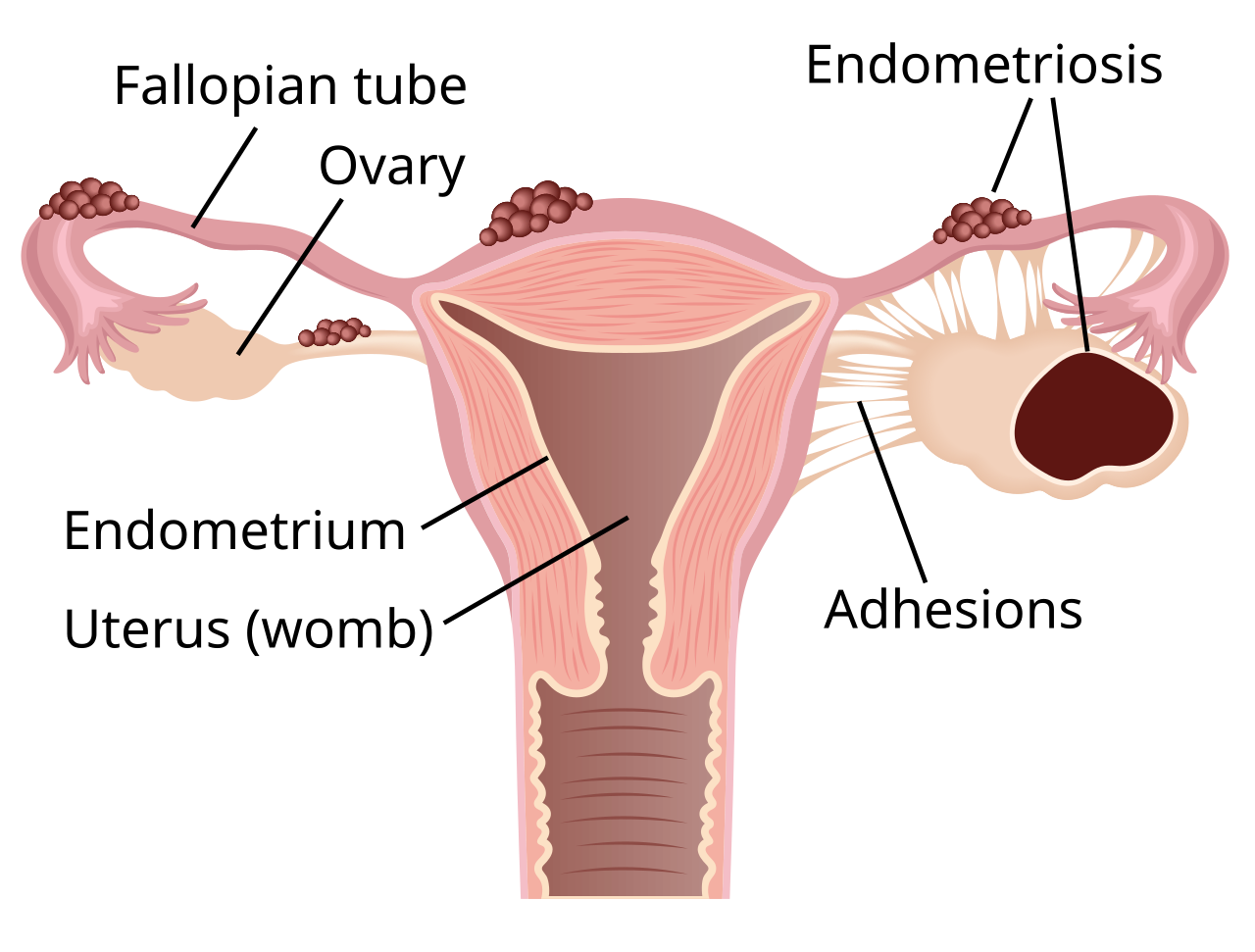
Endometriosis is a complex and often debilitating condition affecting millions globally, characterized by the growth of tissue similar to the uterine lining (endometrium) outside the uterus. These growths, known as implants, lesions, or nodules, react to hormonal changes during the menstrual cycle, leading to inflammation, pain, and sometimes infertility. For those grappling with this condition, the question "La Endometriosis Se Cura?" – meaning "Can Endometriosis Be Cured?" – is often at the forefront of their minds. While a definitive cure remains elusive, significant advancements in understanding and managing endometriosis offer effective strategies to alleviate symptoms, improve quality of life, and address concerns like fertility.Understanding Endometriosis: What It Is and Why It Matters
The journey to managing endometriosis begins with understanding the condition itself. Normally, the endometrium lines the inside of the uterus and is shed during menstruation. In endometriosis, this tissue-like material grows on other organs, most commonly:- On or under the ovaries
- On the fallopian tubes
- Behind the uterus (pouch of Douglas)
- On the ligaments supporting the uterus
- On the intestines or bladder
- Increased Risk: A family history of endometriosis (mother, sister, daughter), periods starting before age 11, short menstrual cycles (under 27 days), and heavy periods lasting more than seven days.
- Decreased Risk: Having been pregnant before, periods starting later in adolescence, and breastfeeding.
- Painful menstrual cramps that tend to worsen over time
- Pain during or after sexual intercourse (dyspareunia)
- Pain in the bowels or lower abdomen
- Heavy menstrual bleeding (menorrhagia)
- Spotting or bleeding between periods
- Gastrointestinal or digestive issues (e.g., diarrhea, constipation, bloating, nausea, especially during menstruation)
- Persistent fatigue or lack of energy
Diagnosing Endometriosis: The Path to Clarity
Accurate diagnosis is the cornerstone of effective endometriosis management. The process typically begins with a thorough discussion of your symptoms and medical history with your healthcare provider. A pelvic exam may reveal tender areas or cysts, but it cannot definitively confirm endometriosis. Imaging tests like ultrasound or MRI can detect larger endometriomas (endometriosis cysts on the ovaries) or deep infiltrative endometriosis, but they are not always conclusive for smaller implants. The gold standard for definitively diagnosing endometriosis remains a minimally invasive surgical procedure called a laparoscopy. During a laparoscopy, a thin tube equipped with a camera and light (laparoscope) is inserted through a small incision near the navel. This allows the surgeon to visualize the pelvic organs directly, identify endometriosis lesions, and often remove them at the same time. While it is a surgical procedure, it provides clear diagnostic confirmation and often immediate therapeutic benefits. The expertise of the surgeon in identifying and excising endometriosis lesions is paramount for both diagnosis and initial treatment.Navigating Treatment Options: Beyond "La Endometriosis Se Cura"
The common query, "La Endometriosis Se Cura?" reflects a natural desire for a definitive end to the suffering. While currently there is no known cure, the focus in medical practice is on comprehensive management to alleviate pain, control disease progression, enhance fertility, and improve overall quality of life. Treatment plans are highly individualized, considering the severity of symptoms, the extent of the disease, and the patient's desire for future pregnancy.Medical Management Strategies
For many, medical treatments are the first line of defense, aiming to manage symptoms by altering hormonal environments or directly addressing pain:
- Pain Relievers: Over-the-counter nonsteroidal anti-inflammatory drugs (NSAIDs) like ibuprofen or naproxen are often recommended for mild pain. For more severe pain, prescription analgesics may be necessary.
- Hormonal Contraceptives: If pregnancy is not desired, hormonal birth control methods such as oral contraceptive pills, hormonal intrauterine devices (IUDs), or contraceptive injections can significantly reduce pain and bleeding by suppressing the growth of endometrial-like tissue and reducing menstrual flow.
- Other Hormonal Medications: For individuals trying to conceive or those with severe symptoms, other medications may be prescribed. Gonadotropin-releasing hormone (GnRH) agonists and antagonists can temporarily induce a menopause-like state, halting the menstrual cycle and causing endometriosis lesions to shrink. While effective, these can have side effects mimicking menopause (hot flashes, bone density loss) and are typically used for a limited duration. Other options include progestin-only therapies. Your doctor will weigh the benefits against potential side effects for your specific situation.
Surgical Management Strategies
When medical treatments are insufficient or if fertility is a primary concern, surgery becomes a viable option. The goal is to remove or destroy the endometriosis implants:
- Laparoscopic Excision Surgery: This is the most common surgical approach for endometriosis. A skilled surgeon meticulously removes all visible endometriosis implants, adhesions, and cysts while preserving healthy tissue. This procedure can significantly reduce pain and improve the chances of pregnancy. However, it's important to understand that new lesions can sometimes regrow, and a combination of surgery with post-operative medical therapy is often recommended for long-term management.
- Hysterectomy: As a last resort for individuals with severe, intractable pain and when childbearing is no longer a consideration, a hysterectomy (removal of the uterus, sometimes along with the ovaries – oophorectomy) may be considered. While this can provide permanent relief from uterine-related pain and bleeding, it is a major, irreversible procedure that ends fertility. It's crucial to have a thorough discussion with your doctor about all implications before considering this option.
Holistic Approaches and Living Well with Endometriosis
Beyond medical and surgical interventions, adopting holistic strategies can play a crucial role in managing endometriosis and enhancing overall well-being.- Dietary Adjustments: Many individuals find relief through an anti-inflammatory diet, rich in fruits, vegetables, lean proteins, and omega-3 fatty acids, while reducing red meat, processed foods, and unhealthy fats.
- Regular Exercise: Moderate physical activity can help reduce inflammation, improve mood, and manage pain.
- Stress Management: Chronic pain can significantly impact mental health. Techniques like mindfulness, yoga, meditation, and deep breathing can help reduce stress and improve coping mechanisms.
- Pelvic Floor Physical Therapy: Endometriosis can lead to muscle tension and dysfunction in the pelvic floor. Specialized physical therapy can help release tension, improve muscle function, and alleviate pain.
- Support Systems: Connecting with support groups, therapists, or counselors can provide emotional validation, practical advice, and a sense of community for those living with chronic pain.